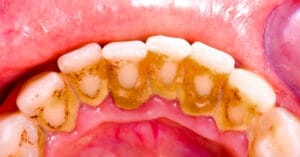
What are the stages of tooth decay, and why does treatment differ at each stage?
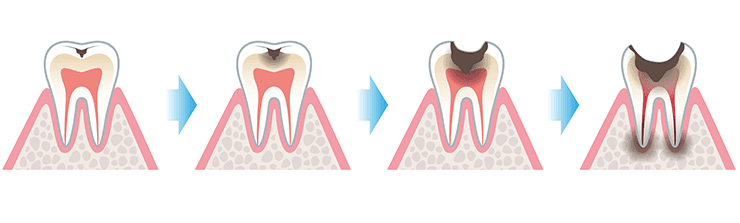
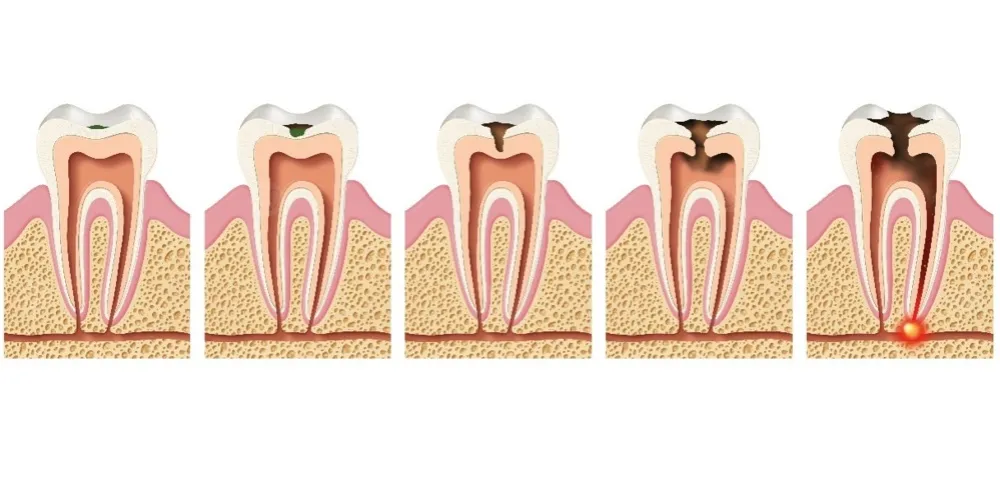
Tooth decay progresses through several gradual stages, starting as a superficial lesion confined to the enamel, then advancing into deeper decay that reaches the dentin and eventually the dental pulp if not treated in time.
In the initial stage, decay appears as white or brown spots on the tooth surface, caused by enamel demineralization due to acids and bacterial activity. At this point, the process can often be halted or partially reversed using fluoride and improving oral hygiene, without the need for a dental filling.
In the second stage, the decay breaks through the enamel and extends into the softer dentin layer. At this stage, the patient may begin to experience sensitivity or mild pain. The tooth typically requires removal of the decayed tissue and placement of a dental filling to restore its structure and protect it.
In more advanced stages, when the decay reaches the tooth’s nerve (dental pulp), it can lead to severe pain or an abscess. In such cases, root canal treatment (endodontic therapy) is usually required, often followed by placing a dental crown. In very late or severe cases, the tooth may be beyond saving and extraction becomes necessary.
This is why the management of tooth decay varies according to its stage. The earlier decay is detected, the simpler, less expensive, and less painful the treatment tends to be. Delayed diagnosis often means the patient will need more complex procedures to preserve the tooth or replace it if it is lost.
Stage One — White Spots (Early Dental Caries)
The first stage of tooth decay is often painless and typically appears as chalky white spots on the tooth surface, especially near the gum line or on areas that are harder to clean.
At this early stage, the enamel begins to lose essential minerals such as calcium due to acids produced by bacteria found in dental plaque. This process is known as enamel demineralization.
Many people notice these white spots on their teeth without realizing that they are an early warning sign of dental caries—a stage at which decay can still be halted and even reversed if managed promptly.
When white spots are detected early, the dentist can treat the initial decay without drilling, using topical fluoride, remineralizing pastes, and by improving daily oral hygiene—such as regular brushing with a fluoride toothpaste and reducing sugar intake.
For this reason, any change in tooth color—particularly the appearance of dull, opaque white spots—should prompt an immediate visit to the dentist to prevent the decay from progressing to deeper, more painful, and more complex stages.
What do white spots on the teeth mean?
White spots on the teeth are the earliest visible sign of initial tooth decay (early dental caries). At this stage, the enamel starts losing minerals, but no actual cavity or hole has formed yet.
These spots usually appear near the gum line or between the teeth and look whiter or chalkier than the surrounding tooth surface. This change is known as “demineralization.”
In this early phase, the damage is still superficial and is usually reversible if treated in time. That’s why noticing white spots is important: it allows for early detection of tooth decay before it progresses to deeper, more complex stages that are harder to treat.
White spot lesions are often linked to poor oral hygiene, frequent intake of sugary foods and drinks, dry mouth (xerostomia), or wearing orthodontic braces without proper cleaning around the brackets and wires.
Can this stage be reversed without drilling?
Yes. At the white spot stage (initial caries), tooth decay can often be reversed without drilling or fillings if it’s detected early and the patient adheres to preventive treatment.
At this point, there is no actual “hole” in the tooth yet. The problem is limited to mineral loss from the enamel surface, which means the enamel can still be strengthened and “re-hardened” using fluoride and improved oral care.
Brushing twice daily with a fluoride toothpaste, using dental floss to clean between teeth, and reducing sugary snacks and drinks between meals can stop the progression of decay and even promote remineralization of the affected area.
The earlier the intervention after white spots appear, the higher the chance of restoring enamel health and preventing progression to more advanced decay that requires drilling and filling.
Best early treatment approaches (fluoride + improved oral care)
The best way to manage the first stage of decay — white spot lesions — is based on two key principles: remineralizing enamel with fluoride and upgrading daily oral hygiene.
Using a fluoride toothpaste with an appropriate concentration, along with a fluoride mouthwash recommended by your dentist, helps strengthen the enamel surface and drive minerals back into the areas where white spots have formed.
Your dentist may also recommend in-office applications of high‑concentration topical fluoride (such as fluoride varnish or gel), or special remineralizing products containing calcium and phosphate compounds (like CPP-ACP and similar formulations).
Improving oral hygiene includes brushing at least twice a day with proper technique, using dental floss or interdental brushes to clean between teeth, and cutting down on sugary foods and carbonated drinks, especially between meals and before bedtime.
Sticking to these measures at the earliest stage of tooth decay greatly increases the chances of halting the process and keeping the teeth healthy, without the need for more invasive treatments later on.
Stage II — Early Enamel Caries (Surface Enamel Lesions) in Line with the Research Intent
In the second stage of dental caries, early enamel lesions become more apparent, typically presenting as a white or brown spot on the tooth surface. At this point, the carious process is still confined to the outer hard enamel layer and has not yet penetrated into the underlying dentin.
During this phase, the accumulation of food debris and fermentable carbohydrates, together with oral bacteria, leads to the production of acids that demineralize and progressively weaken the enamel structure. As a result, the tooth may become more sensitive, especially when consuming sweets or hot and cold drinks.
Early detection of superficial enamel caries allows the dentist to manage the lesion using minimally invasive approaches such as topical fluoride applications or small restorations, thereby preventing progression to deeper, more painful stages of decay.
Accordingly, it is advisable to monitor any change in tooth surface color or the onset of slight surface roughness, while maintaining good oral hygiene by brushing with a fluoride-containing toothpaste and scheduling regular dental check-ups. This helps prevent the progression of surface enamel caries and supports long-term tooth preservation.
How does decay progress from spots to cavities?
In the second stage of dental caries, decay advances from chalky white spots on the enamel surface to the formation of tiny cavities in the tooth.
Acids produced by bacteria in dental plaque continuously attack the outer enamel layer, leading to mineral loss (demineralization) from this hard tissue.
With ongoing plaque buildup and inadequate oral hygiene, the enamel becomes weaker and more porous. As a result, the initial white or brown spots develop into fine, irregular pits on the tooth surface.
At this stage—when decay is still confined to the superficial enamel—these cavities are usually shallow, but they mark the onset of structural breakdown and pave the way for caries to reach the dentin in later stages if left untreated.
Prompt intervention by a dentist at this point is crucial to halt the progression of decay and prevent these small defects from turning into deep, painful lesions.
Does pain appear at this stage?
When caries are limited to the outer enamel layer, patients usually do not experience noticeable pain, since enamel is a hard, non‑sensitive tissue that contains no nerve endings.
Some people may feel very mild sensitivity when consuming cold or sugary foods, but this is often minimal and not bothersome enough to prompt an immediate dental visit.
This is what makes caries in the second stage indirectly dangerous: decay continues to progress silently, with few or no symptoms, until it reaches the more sensitive dentin layer, where it starts to cause clear and sometimes significant pain.
Regular dental check‑ups and simple X‑rays are therefore among the best ways to detect early enamel caries before pain appears, and to treat decay in its initial stages with the least invasive approach possible.
Treating early decay with aesthetic fillings
In the second stage—when decay is confined to the superficial enamel—lesions are usually small and limited, making tooth‑colored composite fillings an ideal treatment option.
The dentist first gently removes the decayed portion of the outer enamel, preserving as much healthy tooth structure as possible.
The small cavity is then prepared and filled with a tooth‑colored restorative material that matches the natural shade of the tooth, restoring its shape and function while protecting it from further spread of decay into the dentin.
Composite fillings are durable, highly aesthetic, and bond well to the enamel, making them an effective treatment for early enamel caries at this stage.
Such timely, minimally invasive treatment preserves the maximum amount of natural tooth structure and prevents the decay from advancing to deeper, more complex stages that would require more extensive—and more costly—procedures.
Stage Three – When Decay Reaches the Dentin Layer
Once dental caries progresses to the dentin layer, symptoms become much more noticeable. This stage marks a turning point, as the lesion advances from a superficial cavity to a deeper, more serious form of tooth decay.
By this point, enough of the enamel has been eroded to expose the underlying dentin, a sensitive tissue rich in fine nerve fibers. As a result, the patient often experiences sudden pain or sharp sensitivity when consuming cold, hot, or sweet foods and drinks.
Dentin caries spreads more rapidly than enamel caries because dentin is softer and more porous than enamel. This porosity allows acids and bacteria to penetrate deeper into the tooth structure, leading to the formation of a visible cavity or hole.
If dentin caries is not treated at this stage—typically by removing the decayed tissue and placing an appropriate dental filling—the inflammation can extend into the dental pulp, causing severe pain and complications that may require root canal treatment (endodontic therapy) or even tooth extraction.
Therefore, stage three caries is a critical warning sign that necessitates immediate consultation with a dentist to halt the progression of decay and preserve the tooth structure before it becomes irreversibly damaged.
Why do teeth suddenly become sensitive?
When dental caries reaches the dentin layer in the third stage, the fine nerve fibers inside the dentin become directly exposed to external stimuli, leading to a sudden onset of tooth sensitivity.
Dentin contains tiny open tubules (dentinal tubules) that are connected to the dental pulp. As the enamel is eroded by decay, these tubules become exposed to air, hot or cold drinks, and even sugary or acidic foods.
So, if you notice a sudden increase in tooth sensitivity while eating or drinking, this may indicate that the decay is no longer confined to the outer enamel, but has advanced into the dentin and is getting closer to the pulp (tooth nerve).
At this stage, ignoring pain or sensitivity allows the decay to progress further, potentially leading to pulpitis (inflammation of the nerve) or a dental abscess. That’s why it’s important to see a dentist promptly to diagnose and treat dentin caries before it develops into more serious stages.
The difference between enamel caries and dentin caries
In the early stages of tooth decay, the damage is limited to the enamel, the hard outer layer that protects the tooth.
Enamel caries typically progresses slowly and may not cause noticeable pain or sensitivity, which is why early detection often depends on regular dental check‑ups.
In the third stage, however, when decay reaches the dentin, the situation becomes more serious.
Dentin is softer and more porous than enamel, so caries spreads through it more rapidly. It also lies much closer to the dental pulp, which is why patients begin to experience obvious pain and sensitivity when consuming food and drinks.
The key difference between enamel caries and dentin caries is the depth of involvement and the presence of symptoms. While enamel decay may progress silently, the extension of decay into the dentin is usually a turning point at which the patient begins to feel pain and sensitivity. This is an important warning sign that calls for immediate treatment to protect the pulp and reduce the likelihood of needing root canal therapy later.
Treatment options (advanced fillings + tooth protection)
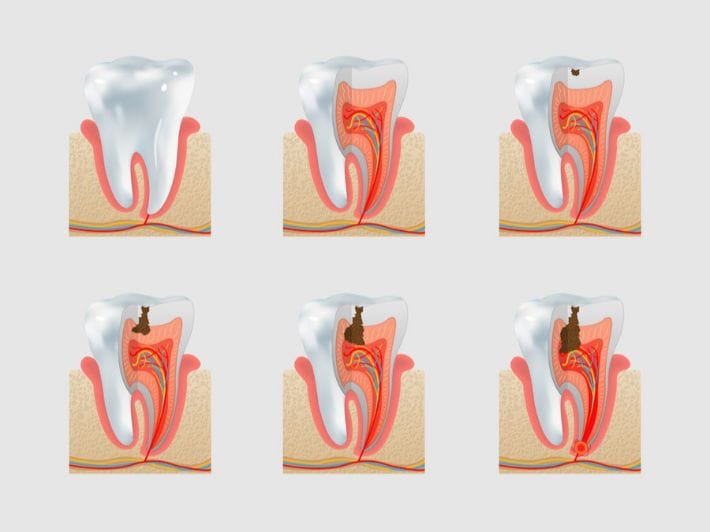
Treating third‑stage caries—when decay has reached the dentin—focuses on removing the decayed dentin and restoring the tooth with an advanced filling that maintains both strength and aesthetics.
Dentists typically use tooth‑colored composite resin restorations or other modern restorative materials, after thoroughly cleaning and disinfecting the carious cavity to ensure no bacteria remain inside the tooth.
In some cases, especially when a large portion of the tooth structure has been lost, an additional protective restoration may be recommended, such as porcelain veneers or full‑coverage crowns, to help distribute biting forces and prevent fracture of the weakened tooth.
Special desensitizing materials can also be applied to seal the exposed dentinal tubules, reduce tooth sensitivity, and protect the pulp from thermal and chemical stimuli.
Following the recommended treatment plan at this stage helps halt the progression of decay, preserve the natural tooth for as long as possible, and avoid reaching the fourth stage, which may require root canal treatment or even extraction of the tooth.
Stage Four – Pulpitis (Inflammation of the Dental Pulp)
In the fourth stage of tooth decay, the carious lesion reaches the dental pulp (the tooth’s nerve), which is the most serious stage because it affects the living part of the tooth that is rich in nerves and blood vessels.
When the pulp becomes inflamed (pulpitis), the patient typically experiences severe, persistent pain that worsens at night and when consuming hot or cold drinks. The pain may radiate to the jaw or ear.
At this stage, a simple dental filling is no longer sufficient. The tooth usually requires root canal treatment (endodontic therapy) to thoroughly clean the root canals from bacteria and inflamed tissue, then fill them and protect the tooth with a dental crown if needed.
Neglecting pulpitis can lead to necrosis (death) of the pulp and the formation of a dental abscess in the gum or the bone surrounding the tooth’s root. This may cause significant swelling and, in advanced cases, may necessitate extraction of the tooth.
Recognizing this stage and seeking prompt dental care when persistent pain appears is crucial to saving the tooth and preventing serious complications.
Symptoms of Deep Decay Reaching the Nerve (Severe Pain, Throbbing, Heat)
When dental caries progresses to involve the pulp (tooth nerve) in the fourth stage of tooth decay, the patient typically begins to experience sharp, sudden pain that may even wake them from sleep.
Many patients describe the pain as throbbing or “pulsating” inside the tooth, especially when lying down or after eating.
The pain is often triggered or worsened by hot or cold food and drinks, and may persist for several minutes even after the stimulus is removed. This pattern suggests pulpitis (inflammation of the dental pulp) rather than simple tooth sensitivity.
In some cases, the pain radiates to the jaw, ear, or head, making it difficult for the patient to pinpoint exactly which tooth is affected.
These symptoms are a clear indication that tooth decay has reached the nerve, and that urgent dental treatment is needed to prevent the condition from progressing to a dental abscess or even loss of the tooth.
When Do You Need Root Canal Treatment?
You need root canal treatment (endodontic therapy) when tooth decay extends into the pulp chamber and causes irreversible inflammation of the nerve tissue.
Key signs that you may require a root canal include: severe continuous or recurring pain, throbbing pain that worsens at night, pain that lingers after consuming something hot or cold, or the appearance of a small swelling (gum boil) on the gum next to the tooth.
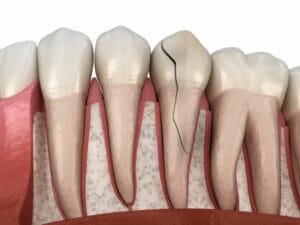
The presence of an abscess or pus around the tooth roots, or a deep fracture that exposes the pulp, also makes root canal treatment necessary to save the tooth and prevent the infection from spreading to the surrounding bone.
At this advanced stage of tooth decay, a simple filling is no longer sufficient, because the pulp is already inflamed or necrotic. The root canals must be thoroughly cleaned, shaped, and filled by a dentist or endodontist.
Can the Tooth Be Saved Without a Root Canal?
At the early stage of pulp irritation, before the inflammation becomes irreversible, the dentist may attempt to preserve the vitality of the pulp by removing deep caries and placing protective liners or a medicated pulp capping material, especially in young patients with decay close to the nerve.
However, once decay reaches the fourth stage and causes acute pulpitis with severe persistent pain or an abscess, saving the tooth without root canal treatment becomes very difficult or no longer medically feasible.
In such cases, root canal treatment is the best option to keep the tooth in the mouth, by removing the inflamed pulp tissue, thoroughly disinfecting the root canals, and sealing them tightly.
Delaying treatment until decay reaches the nerve significantly reduces the chances of preserving the tooth without a root canal, which is why early detection and management in the initial stages of tooth decay is the most effective way to avoid needing a root canal in the future.
Stage Five – Dental Abscess and Tooth Loss
In the fifth stage of dental caries, the damage reaches its most serious level. Decay extends into the dental pulp and root canals, causing severe inflammation that can progress to an abscess in the gums or around the tooth’s root.
At this stage, the patient typically experiences intense, throbbing pain, swelling of the gums or face, marked sensitivity when chewing or consuming hot or cold foods and drinks, along with bad breath and possible discharge of pus around the affected tooth.
If a dental abscess is not treated promptly by a dentist—through appropriate antibiotics and root canal treatment or tooth extraction—the infection may spread to the surrounding bone and soft tissues. This can result in permanent tooth loss and potentially serious complications that affect overall health.
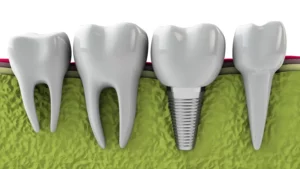
Reaching this advanced stage of tooth decay generally means that a simple filling is no longer sufficient. The tooth often requires root canal therapy or extraction, followed by placement of a dental implant or other prosthetic replacement. This is why early detection and treatment of caries remain the most effective way to protect teeth from abscess formation and eventual tooth loss.
What is a Dental Abscess and Why is it Dangerous?
In the fifth stage of tooth decay, the carious lesion reaches the dental pulp and the tooth root, leading to a build‑up of pus inside or around the tooth roots. This is known as a dental abscess.
A dental abscess is a localized collection of pus caused by a deep bacterial infection within the tooth or in the surrounding gum tissue.
At this stage, decay is no longer confined to the surface of the tooth; it has progressed into the deeper tissues and may cause severe pain, noticeable swelling, and even loss of the tooth if not treated promptly.
The danger of a dental abscess goes beyond losing the affected tooth. Bacteria can spread from the mouth to the jawbone, the paranasal sinuses, and even into the bloodstream, potentially causing a serious systemic infection that endangers overall health.
For this reason, an abscess is considered the most critical stage of tooth decay and requires urgent dental care to prevent complications and protect the remaining teeth and gums.
Symptoms Requiring Immediate Attention
When decay progresses to the stage of abscess formation and tooth loss, a cluster of symptoms may appear that must never be ignored, as they indicate a serious infection inside the mouth.
Key symptoms include: throbbing or constant pain in the tooth or jaw, which worsens when chewing or when the tooth is touched.
You may notice swelling of the gum or cheek near the affected tooth, often with a feeling of fullness or a painful “lump” in the gum.
Another characteristic sign is a bad taste in the mouth or discharge of pus from the gum or around the tooth, accompanied by persistent bad breath.
In more advanced cases, fever may develop, along with general fatigue and difficulty swallowing or fully opening the mouth.
When these symptoms appear in the context of advanced tooth decay, it usually means the condition has reached stage five — abscess formation and tooth loss. At this point, you must see a dentist immediately to prevent loss of the tooth and stop the spread of infection.
Treatment Options (Drainage + Antibiotics + Extraction or Implant)
Treating a dental abscess at stage five focuses on draining the pus, controlling the infection, and preserving the tooth whenever possible.
The first step is usually abscess drainage. The dentist creates a small opening to allow the pus to escape, which relieves pain and reduces pressure in the area.
Afterwards, an appropriate antibiotic is prescribed to treat the bacterial infection and prevent it from spreading to the jawbone or bloodstream, along with pain relievers as needed.
If the tooth can still be saved, the dentist may perform root canal treatment (endodontic therapy) to clean and disinfect the root canals, then fill them and restore the tooth with a crown for protection.
If the tooth is severely damaged or the infection is extensive, tooth extraction may be the safest option to stop the ongoing inflammation.
Following extraction, you can consider replacing the missing tooth with a dental implant or a fixed bridge to maintain your smile, chewing function, and prevent shifting of adjacent teeth.
The choice of treatment plan depends on the stage of decay, the size of the abscess, and the condition of the surrounding bone. That’s why it’s crucial not to delay visiting the dentist when any sign of a dental abscess appears.
How can you tell what stage of tooth decay you’re in?
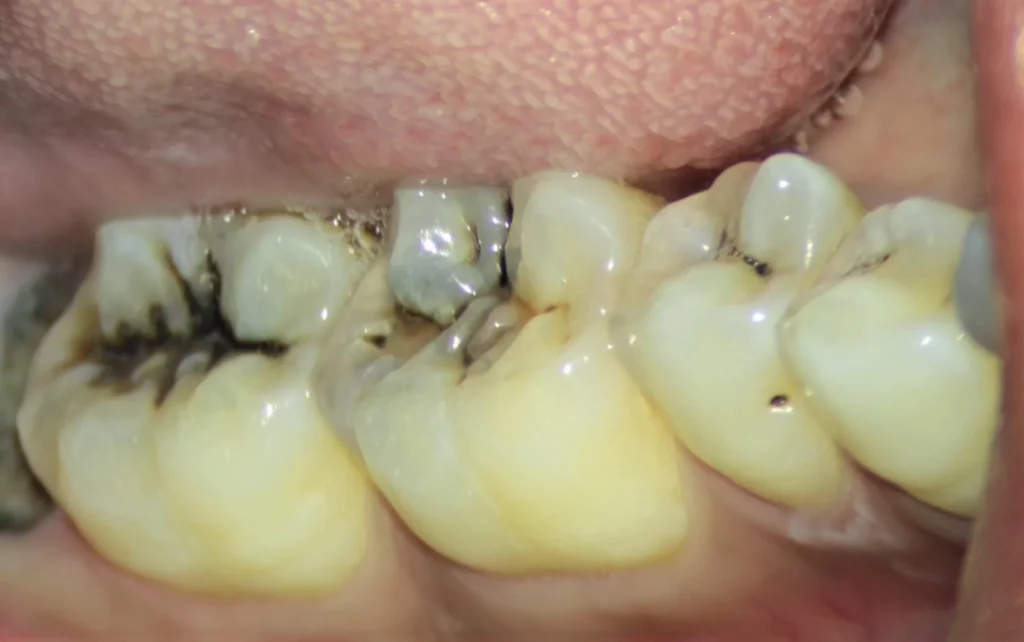
You can get a good idea of how advanced your tooth decay is by paying attention to a set of early and late signs that reflect how deep the cavity has progressed in the tooth.
In the earliest stages, you may notice white or light‑brown spots on the tooth surface without any noticeable pain. At this point, decay is usually superficial and limited to the enamel layer.
As the cavity extends into the dentin beneath the enamel, you may start feeling tooth sensitivity when you eat or drink something cold, hot, or sweet, along with mild, on‑and‑off pain.
If these signs are ignored and decay reaches the tooth’s nerve (the dental pulp), the pain typically becomes more intense, throbbing, and persistent—often worse at night—and may be accompanied by bad breath or an unpleasant taste in the mouth.
In very advanced stages of tooth decay, a dental abscess can form, or you may notice swelling in the gum next to the affected tooth, along with severe pain when chewing or when pressure is applied to the tooth.
Accurately determining the stage of decay requires a clinical examination and dental X‑rays by a dentist. However, recognizing these symptoms can help you gauge whether the cavity is still in its early phase—treatable with a simple filling—or whether it has progressed to a point that may require root canal treatment or more complex procedures.
So, if you notice any change in tooth color, sudden sensitivity, or recurring pain, these are clear warning signs that you are in one of the stages of tooth decay and should see your dentist before the problem worsens.
Why Do Some People Develop Tooth Decay So Quickly?
Many people notice that tooth decay progresses faster for them than for others. This is usually due to a combination of overlapping factors that influence the development of cavities, from the earliest stages until decay reaches the dental pulp (nerve).
Saliva composition and quality play a key role. Reduced saliva flow or changes in its pH lower its ability to neutralize acids and protect tooth enamel, which speeds up the formation of cavities.
Dietary habits are equally important. Diets high in sugars and refined carbohydrates, along with frequent snacking and regular intake of soft drinks and sweetened juices throughout the day, create an ideal environment for bacterial growth and acid production. These acids constantly attack the enamel surface.
Inadequate oral hygiene—such as neglecting regular toothbrushing, flossing, and fluoride use—leads to plaque and tartar (calculus) buildup. This accelerates the progression of decay from the enamel into the dentin and eventually toward the pulp.
Genetic factors and tooth morphology also play a role. Certain people naturally have deeper pits and fissures in their molars, making these areas harder to clean and more prone to cavities.
Additionally, some chronic conditions, such as diabetes, and the use of medications that cause dry mouth (xerostomia), can increase both the risk and speed of tooth decay.
For these reasons, the rate at which cavities develop varies from person to person, depending on lifestyle, oral hygiene practices, overall health, and the inherent characteristics of their teeth. Regular dental check-ups are therefore essential to detect tooth decay at an early stage, before it quickly progresses to more advanced and painful stages.
Complications of Neglecting Dental Caries Treatment
Ignoring dental caries in its early stages can turn a small, easily treatable cavity into serious complications that may threaten both oral and general health.
When tooth decay is left untreated, it gradually progresses from the enamel into the dentin, and eventually reaches the dental pulp (tooth nerve), causing severe pain and persistent sensitivity to hot and cold foods and drinks.
With ongoing neglect, an abscess may form in the gum or at the root apex — a painful collection of pus that can lead to facial swelling and difficulty in chewing and speaking. In advanced cases, the infection can spread to the jawbone or even enter the bloodstream.
Failure to treat dental caries may ultimately result in loss of the affected tooth, necessitating more complex and costly interventions such as dental implants or fixed bridges to replace the missing teeth.
The impact of untreated tooth decay is not limited to the mouth. Medical studies have shown an association between chronic oral infections and an increased risk of cardiovascular disease, diabetes complications, and pregnancy-related problems.
For these reasons, treating dental caries in its early stages and maintaining regular dental check-ups is not just about preserving your smile; it is a key step in protecting your overall health and avoiding complications that are far more difficult to manage than a simple, timely filling.
Special Tips for Preventing Early Childhood Tooth Decay
To prevent early childhood tooth decay and stop it from progressing from superficial white spots to deep cavities, it’s essential to focus on a set of simple, daily habits that are highly effective.
Make sure to brush your child’s teeth twice a day using an age-appropriate amount of fluoride toothpaste. Use a soft-bristled toothbrush and gently clean all tooth surfaces as well as the gum line.
Avoid giving your child a bottle of milk or juice right before bedtime. Sugars that remain on the teeth overnight are one of the main causes of early childhood caries. It’s best to offer water instead.
Limit sweets, biscuits, sugary juices, and soft drinks. If they are given, offer them only after main meals and ensure teeth are brushed afterward, or at least have your child rinse their mouth with water.
Encourage your child to drink water regularly to keep the mouth moist and stimulate saliva flow, which naturally helps clean the teeth and protect against cavities.
It is also important to visit a pediatric dentist every six months to detect and treat any early signs of tooth decay before they progress to pain or dental abscesses.
The dentist may also apply professional topical fluoride or place preventive dental sealants on newly erupted permanent molars to protect them from decay.
By following these simple steps, you can significantly reduce the risk of early childhood tooth decay and support the development of strong, healthy teeth in the long term.
Why Choose Dr. Abeer for Tooth Decay Treatment in Jeddah?
With extensive experience in diagnosing and managing dental caries at all stages, Dr. Abeer is considered one of the leading options for treating tooth decay in Jeddah for patients seeking specialized care and long‑lasting results.
She relies on the latest evidence‑based techniques for managing tooth decay, starting from early detection of initial (incipient) carious lesions, all the way to treating deep caries and restoring teeth with high‑quality aesthetic fillings that preserve both the natural appearance and function of the tooth.
Dr. Abeer also takes the time to explain the stages of tooth decay to each patient step by step, and to outline the most appropriate treatment plan for their specific condition. This helps patients clearly understand their oral health status and make informed decisions about their treatment.
At Dr. Abeer’s clinic in Jeddah, the focus is on providing tooth decay treatment with minimal discomfort, while maintaining strict sterilization protocols, high safety standards, and careful selection of premium restorative materials for fillings and other procedures.
In addition, Dr. Abeer places strong emphasis on caries prevention programs, educating patients on daily oral hygiene and proper home care to prevent future decay. This comprehensive approach makes her clinic an ideal choice in Jeddah for anyone who prioritizes long‑term dental health.