What Is a Lost Dental Filling?
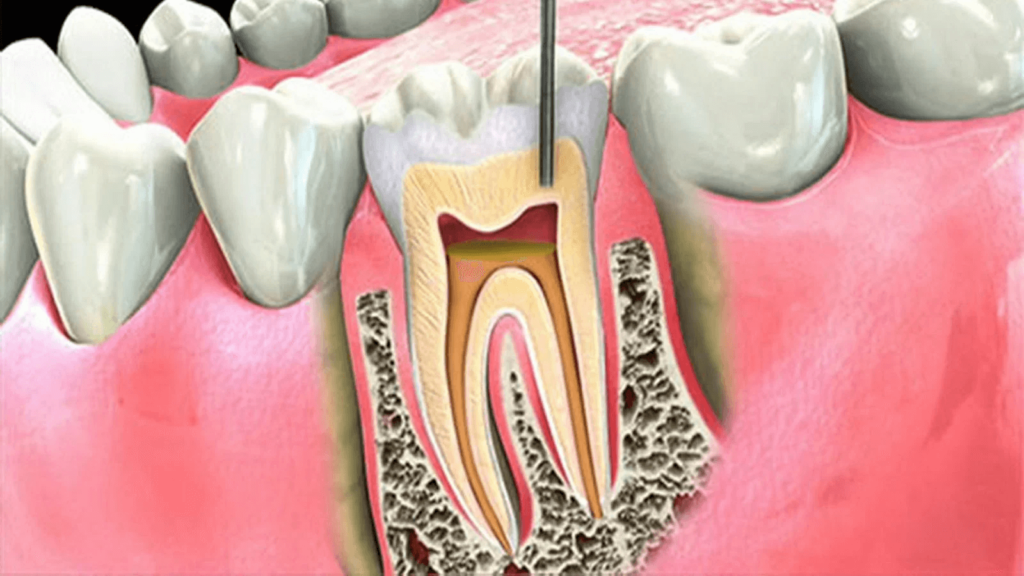
A lost dental filling refers to the dislodgement of a previously placed filling that was used to treat a cavity or a fracture in a tooth or molar, leaving an exposed hollow space inside the tooth.
This usually occurs due to gradual wear of the filling material over time, excessive biting or chewing forces, fracture of the remaining tooth structure, or the development of new decay around the old filling.
When a filling falls out, the patient often experiences sensitivity or pain when consuming cold, hot, or sweet foods and drinks, and may notice a hole or a rough cavity in the tooth with their tongue where the filling used to be.
Although losing a filling is common, it should not be ignored. Leaving the tooth exposed increases the risk of bacterial invasion, progression of tooth decay, and inflammation or infection of the dental pulp (tooth nerve). Therefore, it is important to see a dentist promptly to restore the tooth—either by placing a new filling or replacing the damaged one with a more suitable restoration that protects the tooth over the long term.
Causes of Dental Filling Loss
Filling Wear and Recurrent Decay
Over time, dental fillings can gradually wear down due to constant contact with food and chewing forces. This may create microscopic gaps between the filling and the tooth surface.
These tiny spaces allow food debris and bacteria to accumulate, leading to recurrent caries (decay) beneath the filling, which is one of the main reasons a filling can suddenly fall out.
If decay continues under the restoration, the surrounding tooth structure that supports the filling becomes weakened, causing the filling to lose its stability and eventually become partially or completely dislodged.
Regular dental check‑ups help detect wear and recurrent decay at an early stage, before it progresses to the point where the filling is lost entirely.
Inadequate Cavity Preparation or Poor Bonding
One common cause of filling failure is improper cavity preparation before placing the restoration—for example, not removing all carious tissue or not shaping the cavity in a way that provides proper retention.
Any error during the restorative procedure, such as insufficient drying of the tooth or incorrect use of bonding agents, can also compromise the adhesion between the filling material and the tooth surface.
Poor bonding makes the restoration more prone to loosening over time, especially under strong chewing forces or repeated temperature changes in the mouth.
Meticulous cavity preparation and correct use of adhesive techniques are therefore crucial to prevent early loss of dental fillings.
Excessive Bite Forces and Bruxism
Excessive pressure on the teeth from strong biting forces or the habit of bruxism (night‑time teeth grinding) is a major factor in causing fillings to crack or shift.
Continuous grinding places repetitive stress on the restoration that exceeds its tolerance, particularly in molar fillings that bear most of the chewing load.
Over time, microcracks may develop in the filling or along the tooth margins, allowing bacterial leakage, weakening the restoration’s stability, and eventually leading to its loss.
In such cases, dentists often recommend using a night guard to reduce occlusal forces and protect fillings from fracture or dislodgement.
Chewing Hard Objects and Dental Trauma
Chewing on hard items such as ice, very hard nuts, pen caps, or using teeth to open packages can exert sudden, excessive pressure on fillings.
This can cause the restoration to crack or chip, especially if it is old or already compromised.
Direct trauma to the jaw or teeth—such as from a fall or an accident—may also fracture the filling or the tooth itself, making it easier for the restoration to fall out completely.
Avoiding the use of teeth as tools and steering clear of harmful chewing habits significantly extends the lifespan of dental fillings.
Inappropriate Choice of Filling Material
Selecting an unsuitable filling material for the tooth’s location or the level of chewing forces can directly contribute to filling failure.
For example, using a highly aesthetic but less durable composite in a molar that is subjected to heavy occlusal load may lead to rapid wear or fracture.
Similarly, some restorative materials are not ideal for patients with severe bruxism or those who frequently consume very hard foods.
Choosing the right material requires careful assessment by the dentist of the tooth condition, bite pattern, and how the patient typically uses their teeth, in order to minimize the risk of premature filling loss.
Poor Oral Hygiene
Neglecting regular toothbrushing, flossing, and professional check‑ups increases the risk of decay developing around and beneath fillings.
Plaque and calculus accumulation along the margins of the restoration weakens the tooth structure and leads to marginal caries, creating small gaps that facilitate loosening and loss of the filling.
Poor oral hygiene also promotes gingival inflammation, which over time can affect the stability of the teeth themselves and consequently the restorations they retain.
Maintaining a good oral hygiene routine and attending periodic dental examinations help protect fillings from decay and dislodgement.
Limited Lifespan of Restorations
Every type of dental filling has a specific expected lifespan; after a certain period, the material naturally begins to wear down or develop cracks.
Amalgam (metal) fillings generally last many years, whereas tooth‑colored composite restorations often need replacement sooner, especially in posterior teeth.
Once the restoration exceeds its expected service life, the risk of recurrent caries and loss of adhesion to the tooth increases, making it more likely that the filling will fall out if not replaced in time.
Regular follow‑up with a dentist is essential to assess the condition of older restorations and determine the optimal time to replace them before they fail suddenly and cause pain or tooth fracture.
What Should You Do Immediately If a Dental Filling Falls Out?
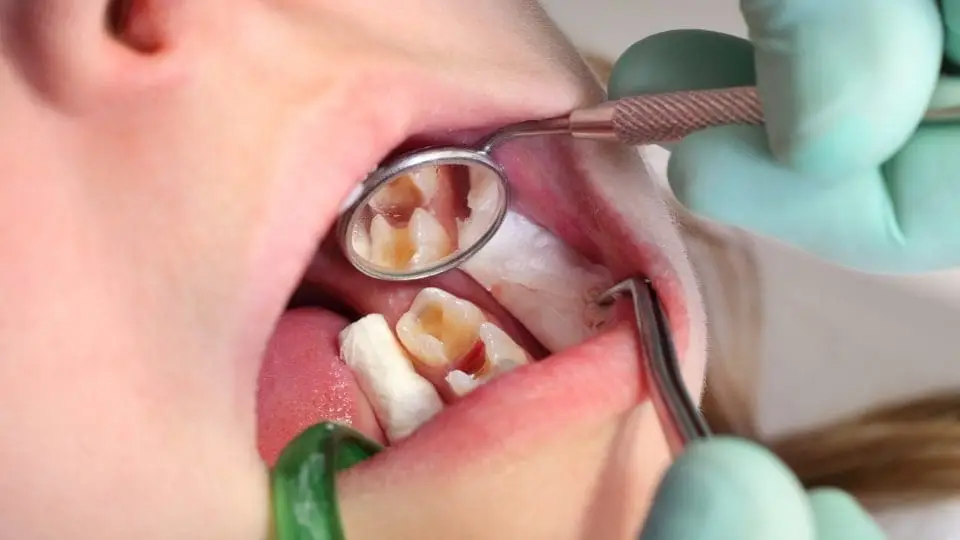
If a dental filling falls out, it’s important to act quickly to prevent pain, complications, and new decay in the exposed tooth.
Start by staying calm and gently rinsing your mouth with lukewarm water to clear away any food debris around the tooth. If you can, keep the filling and bring it with you to the dentist; in some cases, it may help in planning or performing the restoration.
Avoid chewing on the side where the filling is missing, and steer clear of hard, sticky, very hot, or very cold foods and drinks, as they can increase sensitivity in the exposed tooth structure.
You can use an over-the-counter temporary filling material (dental repair kits available in pharmacies) or place a small piece of clean cotton to cover the cavity as a short-term measure. However, this is not a substitute for proper dental treatment.
It’s essential to schedule an urgent appointment with your dentist as soon as possible. Ignoring a lost filling can lead to deeper tooth decay, pulpitis (inflammation of the dental pulp), the need for root canal treatment, or even the placement of a dental crown later on.
Until your appointment, keep the area clean by gently brushing with a soft-bristled toothbrush and carefully using dental floss to reduce bacterial buildup and the risk of infection.
By following these steps promptly, you help protect the tooth and reduce the likelihood of more serious dental problems.
When Does a Lost Filling Count as a Dental Emergency?
A lost dental filling becomes an emergency when it’s accompanied by any of the following:
- Sudden, intense pain
- Marked sensitivity to hot or cold foods and drinks
- Swelling in the gums or cheek
- Bleeding
- Unusual bad breath that may indicate the start of an infection
These signs may mean the dental pulp (nerve) is exposed, or that bacteria have collected in the cavity left by the missing filling, increasing the risk of pulpitis or a dental abscess.
It’s also considered an emergency if:
- A large, old filling falls out completely from a tooth that you rely on for chewing
- Part of the tooth fractures along with the filling, creating a sharp edge that can cut the tongue or cheek
In such situations, you should see a dentist as soon as possible to prevent the problem from worsening.
By contrast, if a small filling falls out without pain or swelling, the visit can usually be delayed slightly—provided you keep the area very clean, avoid chewing on that side, and schedule an appointment to have the filling replaced as soon as reasonably possible.
Treatment options for replacing or repairing a dental filling in line with the research intent
When a dental filling falls out, the dentist has several precise treatment options to either repair the damage or replace the filling in a way that protects the tooth over the long term and provides the best functional and aesthetic outcome.
The process usually begins with a clinical examination and dental X‑rays to determine the extent of decay or any fracture in the tooth structure. The cavity is then thoroughly cleaned to remove any residual caries and remnants of the old filling before placing a new restoration that is appropriate in both type and size.
In many cases, tooth‑coloured restorative materials (composite resin) are preferred, especially for front teeth or areas that are visible when smiling. Metal or amalgam fillings may be used in posterior teeth, where restorations need to withstand high chewing forces.
If the loss of the filling is accompanied by significant structural damage to the tooth or a fracture in the outer walls, the dentist may recommend placing a full‑coverage crown to protect the remaining tooth structure and reduce the risk of future fractures.
When decay has progressed to involve the dental pulp and is associated with severe pain or an abscess, root canal treatment may be required, followed by a permanent restoration or crown to stabilize the tooth and control the spread of infection.
Selecting the most suitable option to replace or repair a filling depends on the dentist’s assessment of the tooth condition, the patient’s age, the tooth’s location in the mouth, and financial considerations. For this reason, it is essential to see a dentist promptly when a filling falls out and not rely on temporary home remedies that may worsen the problem.
Possible Complications After a Filling Falls Out
When a dental filling falls out and is not replaced promptly, this can lead to several bothersome and potentially serious long‑term complications.
If the tooth remains exposed after loss of the filling, food debris and bacteria can accumulate in the cavity, significantly increasing the risk of deep dental caries that may extend into the tooth roots.
The patient may also experience sharp pain when consuming cold, hot, or sugary foods due to pronounced tooth sensitivity following the loss of the filling.
Neglecting treatment can result in pulpitis (inflammation of the dental pulp) and the formation of a dental abscess (purulent infection) around the root, which may require root canal treatment (endodontic therapy) or even tooth extraction in advanced cases.
In addition, the health of the surrounding gingival tissue (gums) can be compromised, leading to gingivitis as a result of the buildup of food remnants and dental plaque in the area where the filling is missing.
For these reasons, seeing a dentist as soon as a filling falls out is essential to prevent these potential complications and to preserve the affected tooth as well as the adjacent teeth.
Ways to Prevent Dental Fillings from Falling Out (Aligned with Search Intent)

To reduce the risk of a dental filling coming loose and to avoid sudden pain, dentists recommend maintaining meticulous oral hygiene. This includes brushing twice daily with a fluoride toothpaste and using dental floss or interdental brushes to remove food debris around the filling.
It is also advisable to avoid biting down on hard foods such as ice and hard nuts, as well as harmful habits like opening packages with your teeth or grinding/clenching your teeth, since these significantly increase the risk of chipping or dislodging the filling.
If you suffer from bruxism (teeth grinding), especially during sleep, it is very important to consult your dentist about getting a night guard. A custom-made night guard helps protect your fillings and prolong their functional lifespan.
Regular dental check‑ups every six months allow your dentist to detect any wear, microleakage, or gaps around the filling early on, and to address them before the filling fails or falls out completely.
Choosing the appropriate type of filling material (such as composite resin, amalgam, or glass ionomer) based on the size and location of the cavity, and ensuring that it is placed correctly by a qualified dentist, are among the most effective strategies to prevent fillings from falling out and to maintain their stability and function for as long as possible.
Post–Filling Care Tips (Optimized for Search Intent)
After a lost dental filling has been replaced, it’s important to follow specific post-treatment care instructions to help the new filling bond properly and to protect the tooth from decay or infection.
Avoid chewing on the treated side for the first 24 hours, especially if you have a composite (tooth-colored) filling or a temporary filling. Stay away from hard and sticky foods such as nuts and chewing gum, as they can dislodge or fracture the new restoration.
Brush your teeth gently using a soft-bristled toothbrush and a fluoride toothpaste. Use dental floss carefully around the restored tooth to avoid pulling on the filling or injuring the gum tissue.
It’s common to experience temporary sensitivity to hot or cold after a filling has fallen out and been replaced. However, if the pain lasts for more than a few days, becomes sharp when you bite down, or you notice a gap, rough area, or change in the bite on the filled tooth, you should see your dentist promptly.
Stick to regular checkups every six months so your dentist can monitor both old and new fillings and detect any problems before a filling fails. Good post-filling care helps extend the lifespan of the restoration, protects the tooth’s nerve (pulp), and reduces the likelihood of needing more complex treatments such as root canal therapy or a dental crown.
When Do You Need a Specialist Dental Evaluation After a Filling Falls Out?
A lost dental filling usually requires prompt professional assessment, especially if you experience sudden tooth pain or marked sensitivity when consuming hot, cold, or sweet foods and drinks.
You should also see your dentist immediately if you notice a fractured part of the tooth, a change in the tooth’s color, or persistent bad breath after the filling comes out. These signs may indicate deep dental caries or pulp inflammation.
Leaving the tooth exposed for an extended period without treatment increases the risk of bacteria reaching the inner tooth structures and can lead to abscess formation or severe pain. In such cases, you may need more complex interventions such as root canal treatment, or even tooth extraction in advanced situations.
For this reason, dental specialists advise against relying solely on temporary home remedies or ignoring a lost filling. It is recommended to book an appointment with a dentist within 24–72 hours to obtain an accurate evaluation and a safe treatment plan that preserves the tooth and prevents complications.
When Should You See a Dentist After a Filling Falls Out, and How Does Dr. Abeer Evaluate Your Case in Line with Your Needs?
When a dental filling falls out, you should book an appointment with your dentist as soon as possible—especially if you notice pain when chewing, sensitivity to hot or cold, or a rough gap that irritates your tongue and traps food debris. Delaying treatment can allow decay to progress deeper or lead to pulp (nerve) inflammation.
At Dr. Abeer’s clinic, the assessment starts with a detailed history of your symptoms and the exact time the filling was lost. This is followed by a thorough clinical examination of the tooth and surrounding gums, along with an evaluation of pain level and thermal sensitivity.
Digital X‑rays are then taken to assess the condition of the pulp, determine how far decay has spread underneath the old filling, and decide whether the tooth only needs a simple replacement filling, a deep filling, root canal treatment, or a crown for additional protection.
This comprehensive assessment helps in selecting the most appropriate type of filling for anterior or posterior teeth, and in providing safe, effective treatment that reduces the risk of the filling dislodging again and preserves your oral health in the long term. This is exactly what most patients are looking for when they search for the causes of filling failure and when they should visit the dentist.