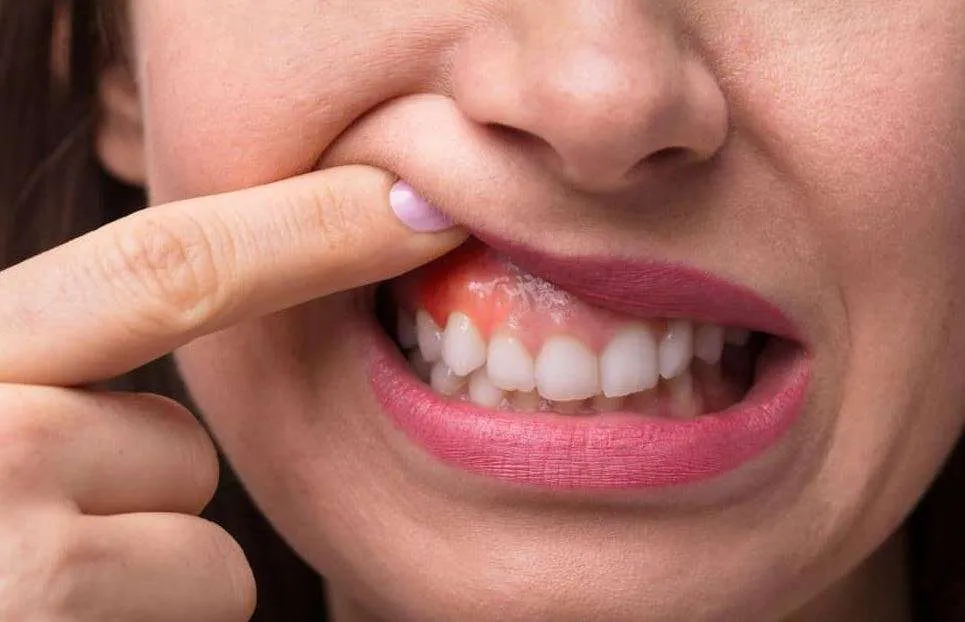
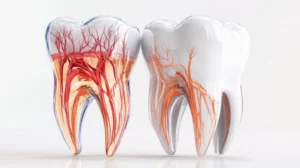
What Is Gum Contouring and Why Is It No Longer Just a Cosmetic Procedure?
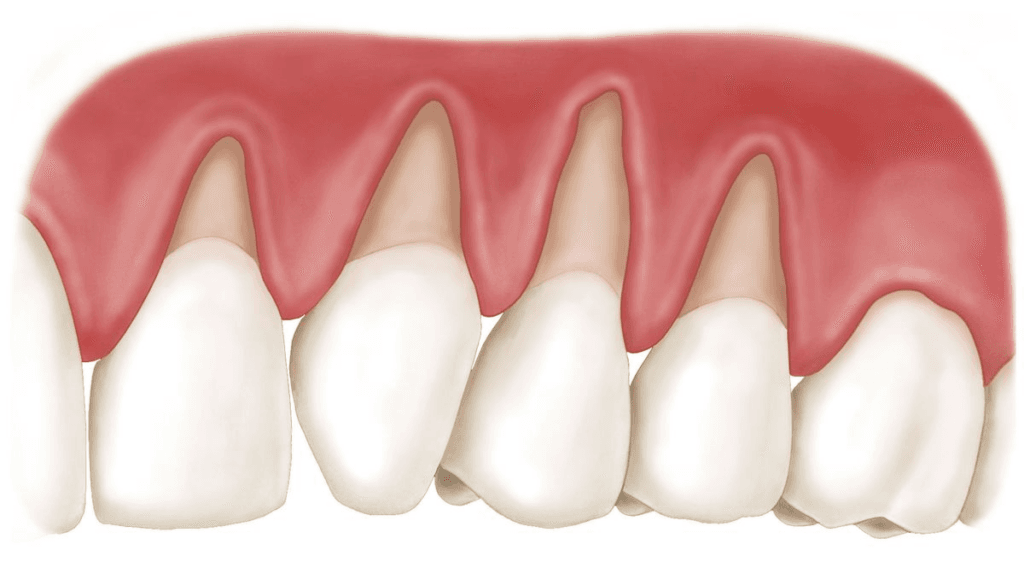
Gum contouring is a relatively simple dental procedure that involves reshaping the gum line around the teeth—by raising it, lowering it, or redesigning its outline—to correct what is known as a “gummy smile” or an uneven gum line.
Today, gum contouring is no longer considered a purely cosmetic treatment. It has become an important part of managing gum disease and maintaining oral health. By exposing more of the tooth structure, it can facilitate the treatment of deep carious lesions and allow for proper placement of crowns and other dental restorations. It also helps improve access for cleaning, reducing the risk of chronic gingival inflammation and periodontal problems.
This procedure not only enhances the appearance of the smile and boosts the patient’s confidence, but also improves tooth function and supports the long‑term stability of the teeth. For these reasons, gum contouring is now regarded as both a therapeutic and functional intervention, in addition to its aesthetic benefits.
When do you actually need to reposition the gums? (Diagnosis matters more than treatment)
Gum Recession and Exposed Tooth Roots
Gum recession is one of the most common conditions that may require actual repositioning of the gums, as it leads to root exposure and bothersome sensitivity when eating or drinking.
Before considering a gum repositioning surgery (such as root coverage procedures) to treat gum recession, the dentist must accurately diagnose the underlying cause: aggressive toothbrushing, calculus (tartar) buildup, chronic gingivitis or periodontitis, or an imbalanced bite (malocclusion).
In some cases, it is sufficient to modify brushing technique, perform deep cleaning (such as scaling and root planing), or adjust the bite before resorting to surgical root coverage and moving the gums back to their natural position.
Choosing the right timing for surgical intervention depends on how much of the root is exposed, the severity of sensitivity, and the risk of losing supporting bone. This is why a precise diagnosis is essential to determine whether gum repositioning is needed now, or if conservative treatment is enough.
Gummy Smile and Excess Gum Display
A gummy smile, where a large area of gum tissue shows when you smile, does not automatically mean you need immediate gum repositioning surgery.
Sometimes, a gummy smile is related to upper lip length, muscle hyperactivity, or jaw position, and not solely to excess gum tissue around the teeth.
Therefore, the dentist starts with a comprehensive smile assessment: measuring tooth length, the amount of visible gum, and the position of the upper jaw, before deciding whether gum repositioning (such as gingivectomy, crown lengthening, or gingival recontouring) is the most appropriate solution.
In mild cases, a minor adjustment of the gum line may be enough to improve the smile. In other cases, the patient may need orthodontic treatment or orthognathic (jaw) surgery. This underscores that identifying the exact cause of a gummy smile is the most important step before choosing any gum repositioning procedure.
Issues Related to Orthodontics or Fixed Restorations
The need for gum repositioning may appear after orthodontic treatment or after placing crowns and fixed bridges, especially when the gum level changes around a particular tooth, or when a tooth looks longer or shorter than its neighbors.
Here, the goal is not just cosmetic. It is also to restore a harmonious gingival contour around the teeth, achieving a balanced smile and a healthy distribution of chewing forces.
Before deciding on gum repositioning, it is crucial to verify that the gum problem is not due to incorrect dimensions of the restoration, overhanging crown margins, or uneven pressure from orthodontic wires.
Treating the root cause first (adjusting the crown, replacing the restoration, or modifying orthodontic movement) is essential. Only then should gum repositioning or reshaping be performed to ensure a stable, healthy result over the long term.
Chronic Gingivitis and Its Effect on Gum Contours
Chronic gingivitis does not only cause bleeding and swelling; over time, it alters the shape of the gingival margins and can lead to periodontal pockets, making teeth appear longer or uneven.
At this stage, some people may think they immediately need gum repositioning to improve the appearance, but the priority is to treat the gingival inflammation itself through deep cleaning, calculus removal, and improved home oral care.
After controlling the inflammation and resolving the swelling, the true contour of the gums becomes clear. Only then can the dentist properly assess the need for gum repositioning, gingival trimming, or pocket correction procedures.
Handled this way, gum repositioning becomes a complementary step to the management of chronic gingivitis, not a substitute for it. This approach preserves the supporting bone and teeth, while providing a more harmonious and stable appearance over the long term.
The real causes of gum problems that require repositioning
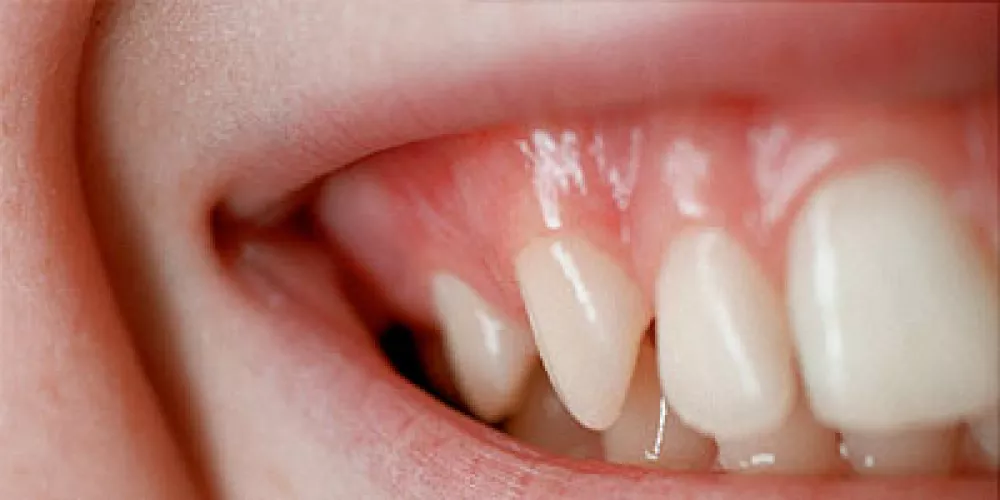
The need for gum repositioning usually arises when there are real, underlying issues affecting the stability of the tooth-supporting tissues, not just a minor superficial problem.
Chronic conditions such as chronic gingivitis and periodontitis lead to loss of the supporting bone around the teeth and recession of the gums. This often makes it necessary to resort to procedures like gum repositioning surgery or cosmetic gum surgery (gingival plastic surgery) to redistribute the gum tissues and cover exposed tooth roots.
Long-standing accumulation of calculus (tartar) and dental plaque, poor oral hygiene, smoking, uncontrolled diabetes, uneven biting forces, and ill-fitting crowns or fillings are all factors that contribute to gum recession and an irregular gum line. As a result, there may be a need for gum repositioning techniques to improve both appearance and function.
In some cases, the cause is genetic, or related to aggressive, incorrect toothbrushing, which gradually wears away the gum tissue.
Understanding the true causes of gum problems helps the dentist determine whether gum repositioning is the appropriate solution, and to choose the optimal treatment plan to maintain the long-term health of the gums and teeth.
Types of Gum Contouring – How to Choose the Right Procedure
Gingivectomy (Removing Excess Gum Tissue)
A gingivectomy is the simplest form of gum repositioning. It is used when there is excess gum tissue covering part of the teeth, making the smile look “gummy.”
In this procedure, the dentist precisely removes the excess gum tissue to create a more even gum line, allowing more of the tooth surface to show and enhancing the appearance of the smile, while maintaining healthy gums.
This option is suitable when your main concern is cosmetic only—for example, when the gums cover part of the teeth without any recession or bone loss.
Gum Contouring (Gingival Recontouring)
Gum contouring, or gingival recontouring, is a more refined step than a simple gingivectomy. Its goal is to harmonize the gum line around each individual tooth.
The dentist may use a laser or surgical instruments to reshape the gum margins in line with the tooth shape and facial features, helping to achieve a more balanced smile and reduce the appearance of a gummy smile.
If your goal with gum repositioning is to improve the symmetry of the teeth and create a straighter, more natural-looking gum line, gum contouring is often the most appropriate procedure.
Gum Grafting (for Recession Treatment)
Gum grafting is a type of gum repositioning specifically designed to treat gingival recession and exposed tooth roots.
The dentist takes a small piece of gum tissue—usually from the palate (roof of the mouth) or from a specialized graft material—and places it over the recessed area to cover the exposed root and reinforce the gum in that region.
If your concern is tooth sensitivity, visible exposed roots, or the risk of tooth loss due to receding gums, gum grafting is likely the treatment that best matches your needs. It is a key part of managing gum recession and improving tooth stability over the long term.
Crown Lengthening
Crown lengthening is a gum repositioning technique used when the visible part of the tooth is too short, or when the dentist needs more tooth structure exposed to place a crown or filling accurately and safely.
During this procedure, a carefully measured amount of gum tissue—and sometimes a small amount of the surrounding bone—is removed to expose more of the tooth surface, while preserving its stability and function.
If you are planning cosmetic treatment such as a perfect smile makeover, or restorative work like crowns or veneers, and the teeth are too short, crown lengthening may be the most suitable gum repositioning procedure to balance aesthetics and function.
How is gum repositioning surgery performed step by step?
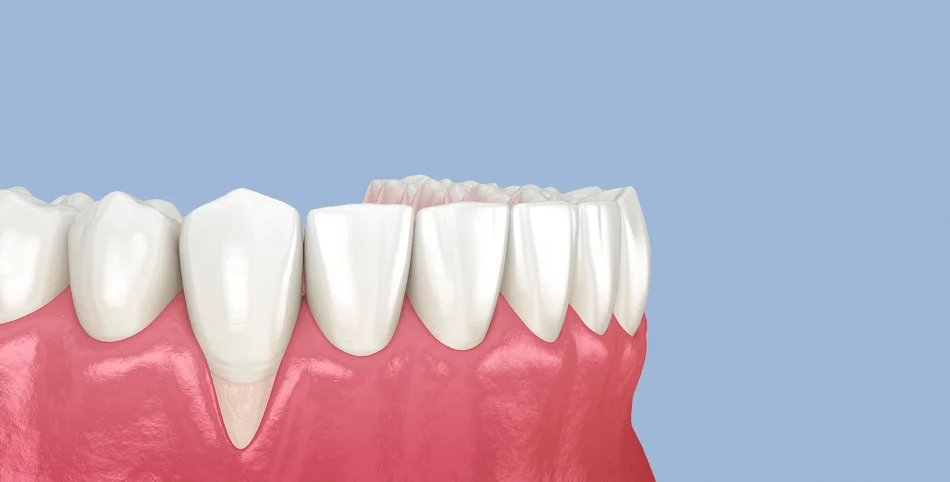
Initial Assessment and Imaging
At the outset of a gum repositioning procedure, the dentist performs a comprehensive initial assessment to evaluate the condition of the gums, teeth, and supporting bone.
The extent of gum recession, the thickness of the gingival tissue, and the presence of any inflammation or periodontal disease that could affect the outcome are carefully assessed.
Conventional X‑rays or 3D imaging (when available) are used to accurately evaluate the bone surrounding the tooth roots and to plan the exact steps of gum repositioning and the path of the gingival flap.
This clinical and radiographic evaluation helps in selecting the most appropriate technique—whether conventional periodontal surgery or laser‑assisted gum repositioning—and ensures that the procedure is carried out safely and effectively.
Anaesthesia and Available Options
Before starting the gum repositioning procedure, the dentist selects the appropriate type of anaesthesia based on the patient’s condition and the extent of the intervention.
Local anaesthesia is most commonly used to numb the area of the gums to be repositioned so that the patient does not feel pain during the surgery.
In some cases—particularly for patients with significant dental anxiety—mild sedatives or intravenous (IV) sedation may be used alongside local anaesthesia.
Choosing the type of anaesthesia is a key part of the treatment plan for gum repositioning and is discussed with the patient in advance to ensure maximum comfort and safety throughout the procedure.
Performing the Procedure (Laser or Conventional Surgery)
Once adequate anaesthesia has been achieved, the gum repositioning procedure is carried out according to the pre‑established treatment plan.
In conventional periodontal surgery, the dentist makes a precise incision in the gum to create a gingival flap that can be mobilised, then gently separates the gum tissue from the bone to allow coverage of the exposed root surface.
In laser‑assisted gum repositioning, a focused laser beam is used to incise the tissue with higher precision and reduced bleeding, while preserving as much healthy tissue as possible.
The gums are then advanced or repositioned to cover the targeted portion of the tooth. When needed, soft‑tissue grafts or biomaterials may be used to reinforce the area and increase tissue thickness.
The choice between laser and conventional surgery depends on the clinical status of the gums, the clinician’s expertise, and the equipment available in the practice; both approaches aim to achieve the best possible functional and aesthetic outcome.
Wound Closure and Follow‑up
At the end of the gum repositioning procedure, the dentist secures the gums in their new position, usually using fine, mostly resorbable sutures.
Wound closure is performed carefully to stabilise the tissue, promote rapid healing, and minimise the risk of bleeding or infection.
A periodontal dressing may be placed temporarily to protect the surgical site during the first few days.
The patient then receives detailed post‑operative instructions, including how to clean the teeth and gums, what foods are preferable, and how to take prescribed analgesics or antibiotics if indicated.
Follow‑up appointments are scheduled to monitor healing, remove non‑resorbable sutures if present, and assess gum stability and the success of the repositioning in the short and medium term.
Recovery After Surgery — The Key to a Successful Outcome
The healing phase after a gum repositioning (gum graft / gingival repositioning) procedure is the most critical step to ensure that the gums remain stable around the teeth and that you achieve a long-lasting functional and aesthetic result.
Dentists strongly recommend strictly following all post‑operative care instructions, such as avoiding chewing on the surgical side and sticking to soft, cool foods during the first few days. This helps protect the grafted or repositioned gum tissue.
Maintaining excellent oral hygiene is also essential. In the beginning, you should brush with a soft‑bristled toothbrush while avoiding the surgical area, and use an antiseptic mouthwash prescribed by your dentist to reduce bacterial load and promote faster gum healing.
Refraining from smoking and avoiding touching the graft site with your tongue or fingers play a major role in stabilizing the gingival graft and reducing the risk of infection or graft failure.
Regular follow‑up visits with your dentist throughout the recovery period after gum repositioning surgery allow early detection of any complications and timely intervention. This helps maintain stable gum levels around the teeth and preserves the esthetic and health results over the long term.
Alternatives to Gum Repositioning – Can Surgery Be Avoided?
In many cases, non-surgical options can be tried before deciding on surgical gum repositioning, especially when gum recession is still in its early stages.
Key alternatives include modifying toothbrushing habits by using a soft-bristled toothbrush and gentle brushing techniques to minimize gum irritation, along with using toothpaste formulated for sensitive gums and a mouthwash containing anti-inflammatory agents.
Your dentist may also recommend professional deep cleaning (scaling and root planing) to remove plaque and tartar deposits from below the gumline. This can help halt the progression of gum recession and may reduce the need for surgery.
In some situations, cosmetic fillings or restorative materials are placed to cover exposed tooth roots, improving appearance and reducing sensitivity as a temporary alternative to gum repositioning.
However, when recession is advanced or a large portion of the tooth roots is exposed, gum repositioning surgery or gum grafting often becomes the most effective treatment to protect the teeth in the long term.
Ultimately, the dentist will choose the most appropriate approach—whether non-surgical measures or gum repositioning surgery—based on the severity of gum recession, the condition of the supporting bone, and accompanying symptoms such as sensitivity or gum pain.
Gum Repositioning Cost — What Determines the Price?
The cost of gum repositioning varies from one patient to another, depending on several key factors that directly influence both the price and the treatment plan.
The primary factor is the nature of the gum problem. There is a clear difference between repositioning the gums to treat gum recession and cover exposed tooth roots, and performing the procedure purely for cosmetic reasons to improve a “gummy smile.”
The overall complexity of the case and the number of teeth requiring gum repositioning also play a major role in calculating the cost. The price increases as more teeth are involved, or if the patient needs a gingival graft, or if advanced microsurgical techniques are used.
The periodontist’s level of expertise and how well the clinic is equipped can also affect the price, especially when modern technologies such as surgical lasers or 3D imaging systems are used.
In addition, fees differ from one clinic to another and from one city to the next, depending on the clinic’s reputation, sterilization standards, and the quality of postoperative follow-up.
Ultimately, the exact cost of gum repositioning is determined after a clinical examination, appropriate dental imaging, and the development of a personalized treatment plan that clearly explains all expected fees before starting the procedure.
When should you contact your dentist immediately after the procedure?
After a gingival repositioning (gum repositioning) surgery, you should contact your dentist or periodontist right away if you experience heavy bleeding that does not stop with gentle pressure after 20–30 minutes, or if you notice increasing swelling of the gums or face accompanied by severe pain that does not improve with the prescribed painkillers.
Fever, discharge of pus, a foul odor from the surgical site, or the gums turning markedly darker in color with a throbbing sensation are all warning signs of inflammation or infection that require urgent evaluation.
You should also call your doctor immediately if you develop persistent numbness in your lips or gums after the local anesthetic should have worn off, or if you have difficulty swallowing or breathing, or notice that the protective dressing or sutures have come loose or shifted from their position.
Early follow‑up with your dentist after gum repositioning surgery helps prevent serious complications, speeds up wound healing, stabilizes the gums, and protects the tooth roots over the long term.
Book Your Consultation with Dr. Abeer and Start a Treatment Plan Tailored to Your Needs and Search Intent
Schedule your consultation now with Dr. Abeer, a specialist in managing gingival mobility and correcting gum recession, to develop a personalized treatment plan that matches your condition and your goal of finding the most effective, pain‑free gum treatment with long‑lasting results.
During the consultation, Dr. Abeer will carefully examine your gums and teeth, assess the degree of gum mobility or recession, and explain the available treatment options—such as gum grafting, surgical or laser-assisted repositioning of the gums, or conservative, minimally invasive approaches in early cases.
You will receive a clear, easy‑to‑understand explanation of each step of the treatment, expected healing time, estimated cost, and customized post‑procedure gum care instructions to help stabilize the results and prevent the problem from recurring.
If you’re looking for a solution to gum mobility, effective treatment for gum recession, or aesthetic enhancement of your smile while protecting your tooth roots, booking a consultation with Dr. Abeer is the first safe, evidence‑based step toward a suitable treatment plan grounded in accurate diagnosis and the latest medical standards.