Table of Contents
What Is a Posterior Open Bite?
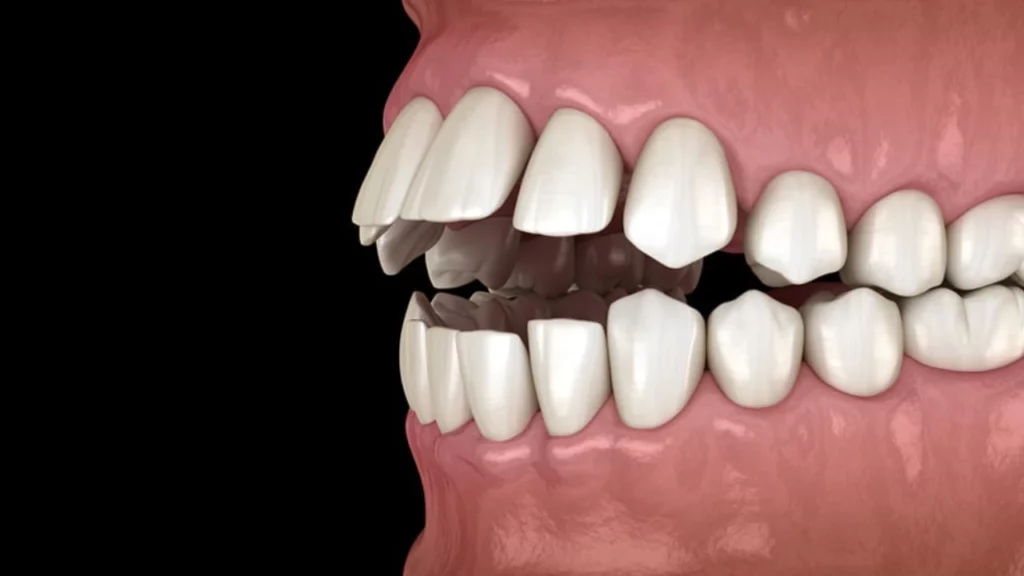
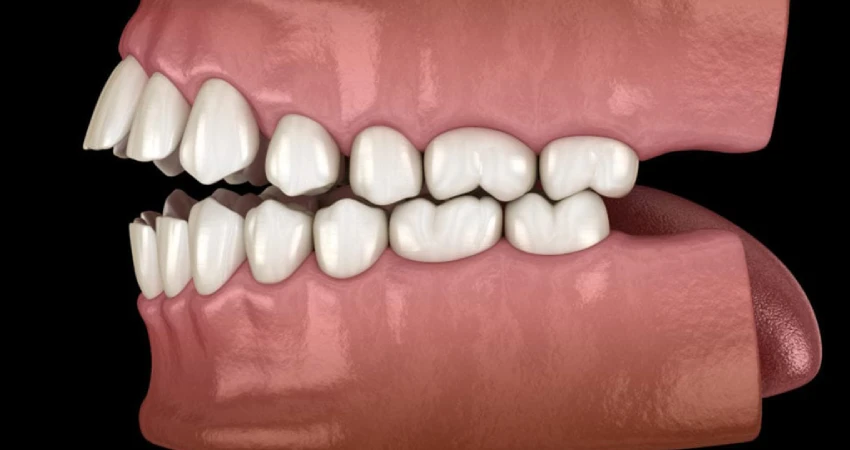
A posterior open bite is a type of malocclusion in which the upper and lower teeth on one or both sides of the mouth do not make contact when the jaws are closed. As a result, a visible gap remains between the back teeth, even though the front teeth (incisors) come together normally.
This condition most commonly affects the premolars and molars, and it can compromise chewing efficiency and occlusal stability. Patients may have difficulty grinding food properly, and biting forces are not distributed evenly between the two sides of the jaw.
Posterior open bite is a relatively common orthodontic problem and is associated with several contributing factors, such as harmful oral habits, disturbances in jaw growth, or abnormal tooth eruption patterns. It requires thorough diagnosis and a comprehensive treatment plan by an orthodontist to preserve long‑term oral health and function.
Main Causes of Posterior Open Bite
A posterior open bite develops as a result of several factors that affect jaw growth and tooth position. Harmful oral habits during childhood are among the most common causes, such as prolonged thumb sucking, tongue thrusting between the teeth during swallowing or speaking, or extended use of pacifiers beyond the medically recommended age.
Genetic factors also play a significant role, as a child may inherit a particular jaw shape or growth pattern that increases the likelihood of poor contact between the upper and lower teeth at the back of the mouth.
In addition, certain chronic breathing problems—such as nasal obstruction or enlarged tonsils and adenoids—can lead to habitual mouth breathing. Over time, this alters tongue posture and jaw position, contributing to the development of a posterior open bite.
Temporomandibular joint (TMJ) disorders, loss of posterior teeth without proper replacement, and untreated malocclusion can also be involved in the onset and progression of this condition. For these reasons, early diagnosis and timely intervention by a dentist or orthodontist are essential to prevent the problem from worsening.

Symptoms and Complications of Posterior Open Bite
A posterior open bite can lead to a range of functional and aesthetic problems that impact oral health and overall quality of life.
One of the most common issues is difficulty biting and chewing on the sides, because the upper and lower posterior teeth do not make proper contact. As a result, patients tend to rely excessively on their front teeth or chew on one side only.
Patients may also experience speech disturbances, particularly with sounds that require a tight seal between the teeth. This can cause a lisp or allow excess air to escape while speaking.
From an aesthetic standpoint, visible gaps may appear between the back teeth when smiling or opening the mouth, and the jaw may look tilted or asymmetrical. These changes can be a source of embarrassment and may lower self‑confidence.
Over time, a posterior open bite can cause uneven tooth wear and pain in the temporomandibular joint (TMJ), which may present as pain in front of the ear, clicking or popping when opening and closing the mouth, and headaches. It can also increase the risk of gingivitis and food impaction in the spaces between the teeth.
If left untreated, these symptoms often worsen. For this reason, it is advisable to consult a dentist or orthodontist if any of these signs are noticed.
How Does a Dentist Diagnose a Posterior Open Bite?
Diagnosing a posterior open bite at the dentist or orthodontist begins with taking a detailed medical and dental history, with a special focus on oral habits such as thumb sucking, tongue thrusting, or swallowing difficulties, and asking about any problems with speech or chewing.
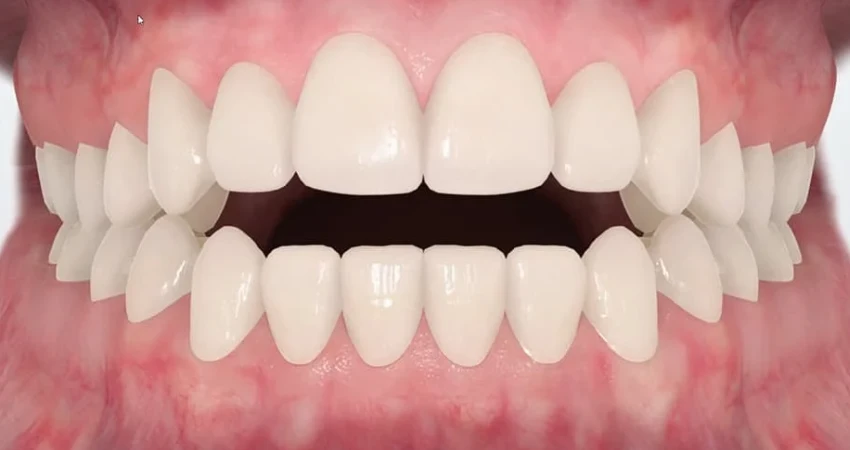
The clinician then performs a thorough clinical examination of the mouth and jaws. When the teeth are brought together, they look for a gap between the upper and lower teeth on the sides instead of the normal contact, and they assess tongue posture, tooth angulation, and the patient’s craniofacial growth pattern.
Diagnosis of a posterior open bite also relies on dental radiographs such as panoramic X‑rays and lateral cephalometric radiographs to evaluate the relationship between the jaws, the direction of jaw growth, and the presence of any skeletal abnormalities.
The dentist may also request dental impressions or a three‑dimensional digital scan to create a model of the jaws, which helps in accurately analyzing the malocclusion and planning treatment for the open bite.
This comprehensive diagnostic approach makes it possible to distinguish between an anterior and a posterior open bite, and to identify whether the underlying cause is skeletal (related to jaw bone structure) or functional (related to harmful oral habits), thereby guiding the choice of the most appropriate treatment plan.
Orthodontic Treatment Options for Children and Adolescents
Managing lateral open bite in children and teenagers relies mainly on early orthodontic intervention to correct the bite and guide jaw growth before skeletal maturity.
The orthodontist may use functional appliances, clear aligners, or conventional fixed braces (metal brackets and wires) to redirect jaw growth and move the posterior teeth upward or forward, achieving proper interdigitation between the upper and lower jaws.
In some cases, special appliances are used to stop harmful oral habits such as thumb sucking or tongue thrusting, as these are among the most common causes of lateral open bite in children.
Every orthodontic treatment plan is individually tailored after reviewing radiographs and performing clinical examinations. The plan may involve maxillary expansion, fixed orthodontic treatment, or a phased approach that starts with a simple appliance and is later completed with conventional braces.
Orthodontic treatment at this developmental stage helps reduce the need for future surgical intervention, improves chewing and speech function, and enhances the overall appearance of the smile, which in turn boosts the child’s or adolescent’s self‑confidence.
Treatment options for adults
Treatment options for posterior open bite in adults vary according to the severity of the condition and its underlying cause. They often include orthodontic treatment with fixed appliances or clear aligners to realign the teeth and improve the occlusion, sometimes combined with precisely placed elastics to guide the movement of the posterior teeth and help close the gap between the jaws.
In more complex or advanced cases of posterior open bite in adults, orthognathic surgery may be recommended, in a coordinated approach between the orthodontist and the oral and maxillofacial surgeon, to reposition the maxilla, the mandible, or both. This can create better harmony between the jaws and improve both function and facial aesthetics.
Mini-implants or temporary anchorage devices (TADs) may also be used to provide stable anchorage and allow controlled tooth movement without compromising adjacent teeth. This is particularly effective in open bite cases related to malposition of the posterior teeth.
It is also essential to address detrimental oral habits such as tongue thrusting or mouth breathing through targeted exercises or orofacial myofunctional therapy. This helps maintain the stability of posterior open bite correction in adults and reduces the likelihood of relapse.
Tips to Prevent Worsening of a Lateral Open Bite
To prevent a lateral open bite from getting worse and to protect the health of your teeth and jaws, it is essential first to stop harmful oral habits such as thumb sucking, nail biting, and tongue thrusting between the teeth. These habits are among the main causes of malocclusion and the persistence of an open bite.
Make sure to follow up regularly with an orthodontist who has experience in treating lateral open bite, and strictly adhere to wearing braces and retainers according to the treatment plan. Skipping appointments or not wearing the prescribed appliances can lead to relapse or even worsening of the condition.
Try to chew food evenly on both sides of the mouth, and avoid extremely hard or sticky foods that may put excessive pressure on the teeth and compromise treatment results. It is also advisable to cut food into small pieces to make chewing easier and more controlled.
Pay attention to your mouth and tongue posture during rest and speech. The mouth should be kept closed as much as possible, with the tongue resting against the palate (roof of the mouth), not between the teeth. Your dentist may recommend specific tongue exercises or myofunctional therapy to improve swallowing patterns and reduce tongue pressure on the front and side teeth.
Maintain excellent oral hygiene using a toothbrush, fluoride toothpaste, and dental floss, as gum disease or tooth wear can aggravate malocclusion and compromise the stability of lateral open bite treatment.
Finally, if you notice difficulty chewing, changes in how your teeth come together, or pain in the temporomandibular joint (TMJ), consult your dentist or orthodontist early. Timely evaluation allows adjustments to the treatment plan before the open bite progresses and requires more complex interventions.
Lateral Open Bite Treatment in Jeddah with the Expertise of Dr. Amir Ghiyath Al‑Zahrawi
At Dr. Amir Ghiyath Al‑Zahrawi’s center in Jeddah, patients receive advanced, evidence‑based care for lateral open bite using state‑of‑the‑art orthodontic techniques and fully digital planning of tooth and jaw movements.
Dr. Amir relies on an accurate, comprehensive diagnosis of each lateral open bite case, using 3D radiographic imaging and thorough clinical examination to identify the underlying cause—whether it is dental malocclusion, skeletal jaw discrepancies, or harmful oral habits.
Based on this assessment, an individualized treatment plan is designed for every patient. This may involve clear aligner therapy, fixed orthodontic appliances, functional orthopedic devices, or, in more severe cases, coordinated orthognathic (jaw) surgery to optimize lateral occlusion as well as chewing efficiency and speech function.
The primary goals of lateral open bite treatment at Dr. Amir Ghiyath Al‑Zahrawi’s clinic in Jeddah are to establish a healthy, stable bite, enhance smile aesthetics, and prevent complications such as tooth wear and temporomandibular joint (TMJ) pain, with meticulous follow‑up to ensure long‑term stability of the results.

FAQs About Posterior Open Bite
What is a posterior open bite?
A posterior open bite is a condition where the back teeth do not touch when the mouth is closed, creating a gap between the upper and lower teeth.
What causes posterior open bite?
Common causes include thumb sucking, tongue thrusting, jaw growth issues, mouth breathing, and missing teeth.
Is posterior open bite serious?
Yes, if untreated, it can lead to chewing difficulties, speech problems, jaw pain, and long-term dental complications.
How is posterior open bite treated?
Treatment may include braces, clear aligners, functional appliances, or surgery in severe cases.
Can posterior open bite be corrected without surgery?
Yes, mild to moderate cases can often be treated with orthodontic appliances without surgery.
Does posterior open bite affect speech?
Yes, it can cause speech issues such as lisping or air leakage during pronunciation.
At what age should posterior open bite be treated?
Early treatment in children is ideal, but it can still be treated effectively in adults.
Can posterior open bite come back after treatment?
Yes, relapse is possible if retainers are not used or harmful habits continue.