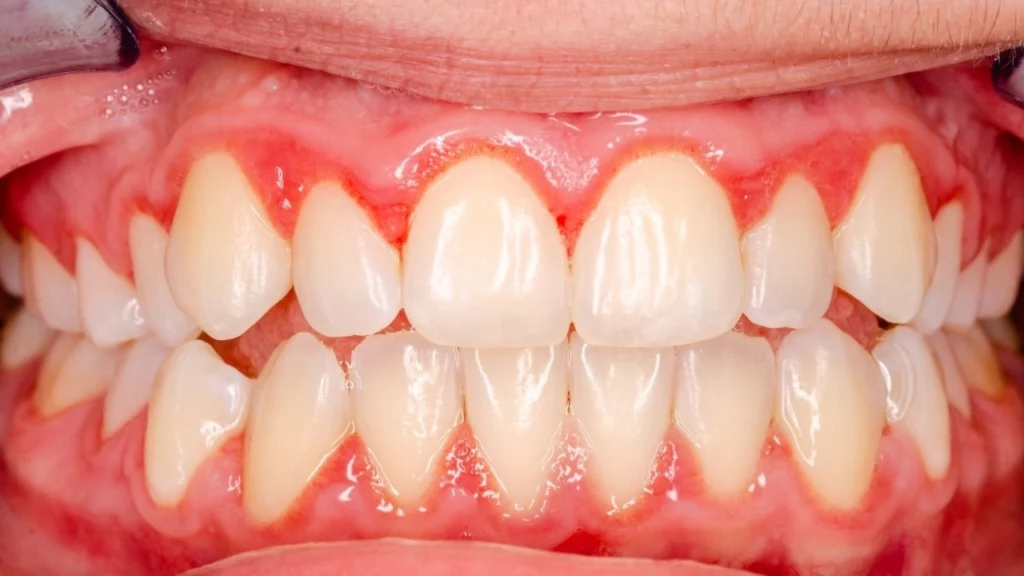
Chronic gingivitis is a common form of gum disease characterized by persistent inflammation of the gum tissues surrounding the teeth. It typically develops due to the long-term accumulation of plaque and bacteria along the gumline. If left untreated, chronic gingivitis may progress to more severe periodontal disease, leading to gum recession, bone loss, and eventually tooth loss. Understanding the causes, symptoms, and treatment options of chronic gingivitis is essential for protecting both oral health and overall wellbeing.
Table of Contents
What is Chronic Gingivitis?
Chronic gingivitis is a long‑standing inflammatory condition affecting the gum tissue surrounding the teeth. It most commonly develops as a result of the buildup of dental plaque, calculus (tartar), and bacteria on the tooth surfaces and below the gumline.
This form of gum disease is characterized by persistent redness, swelling, and bleeding of the gums, especially during toothbrushing or flossing, and it tends to continue in the absence of timely, effective treatment.
Over time, chronic gingivitis can progress to periodontitis, a more serious stage of gum disease that may lead to gum recession, loosening of the teeth, and, in advanced cases, tooth loss.
Several factors can increase the risk of developing chronic gingivitis, including poor oral hygiene, smoking, diabetes, hormonal changes, and compromised immune function.
Regular dental check‑ups, professional teeth cleaning, and consistent daily oral care using a toothbrush, dental floss, and antimicrobial mouthwash are the cornerstone of preventing chronic gingivitis and limiting its impact on oral health.
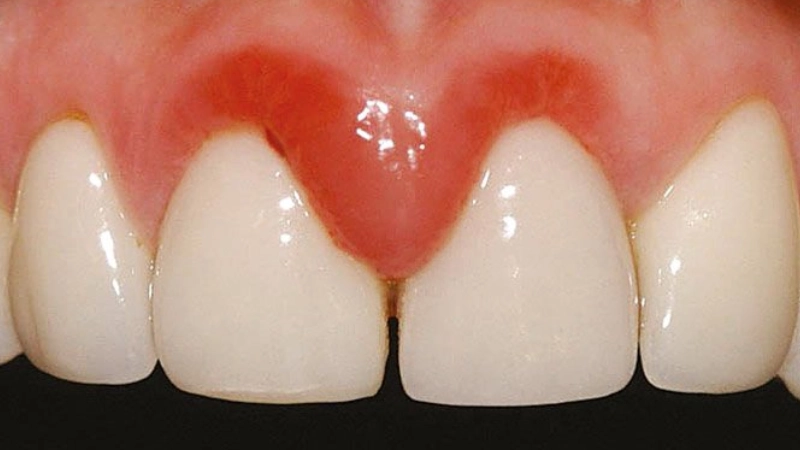
Main Causes of Chronic Gingivitis
Chronic gingivitis usually develops as a result of plaque and tartar buildup around the teeth due to poor daily oral hygiene. This allows bacteria to spread toward the gums and trigger persistent inflammation.
Unhealthy habits such as smoking play a major role as well; smoking impairs blood circulation in the gums and reduces their ability to fight infection, which significantly increases the risk of chronic gum disease.
Chronic systemic conditions like diabetes, cardiovascular disease, and immunodeficiency are also important contributors, as they weaken the body’s defense mechanisms and accelerate the progression of gum inflammation.
In addition, poor nutrition and vitamin deficiencies—especially vitamin C—can compromise gum tissues, making them more prone to bleeding and chronic inflammation.
Hormonal factors in women during pregnancy, puberty, or menopause should not be overlooked, since hormonal fluctuations can increase gum sensitivity and tendency to become inflamed.
Poorly fitted dental restorations (such as fillings, crowns, and bridges), as well as excessive bite forces from teeth grinding (bruxism), can further irritate the gums and perpetuate long‑standing inflammation.
All of these factors combined highlight the importance of maintaining proper oral hygiene and visiting the dentist regularly to prevent chronic gingivitis and treat it in its early stages.

Common Symptoms That May Indicate Gum Inflammation (Gingivitis)
People with chronic gingivitis often experience a recurring set of symptoms that signal an ongoing inflammatory process requiring early intervention.
One of the most noticeable signs is redness and swelling of the gums. The gums appear darker than their normal pink color, look puffier, and feel tender or uncomfortable when touched.
Bleeding gums during toothbrushing or when using dental floss is another hallmark sign, especially if it happens frequently or on a daily basis.
Many patients also complain of persistent bad breath (halitosis) despite maintaining good oral hygiene, which is strongly associated with chronic gum inflammation.
Some may experience mild pain or a throbbing sensation in the gums, along with itching or discomfort when consuming hot or cold foods and drinks.
In more advanced stages, changes in gum contour may be observed, such as gum recession (pulling away from the teeth) or the development of pockets and gaps between the teeth and gums. These spaces trap more dental plaque and calculus (tartar), accelerating the progression from simple gingivitis to more serious periodontal disease.
The presence of these symptoms warrants prompt evaluation by a dentist or periodontist to prevent the complications of chronic gum inflammation on both oral health and overall systemic health.
Complications of Neglected Gingivitis on Oral and General Health
Leaving chronic gingivitis untreated doesn’t just harm your teeth and gums; it can also affect your overall health.
When gum inflammation persists without proper care, it may progress to periodontitis, leading to gum recession, formation of deep periodontal pockets, loss of the bone supporting the teeth, and eventually tooth mobility or even tooth loss in advanced stages.
Chronic gum infection and inflammation can allow bacteria to enter the bloodstream, increasing the risk of cardiovascular diseases, hypertension, and poor blood sugar control in people with diabetes.
Long‑standing periodontal disease has also been linked to a higher likelihood of preterm birth and low birth weight in newborns, in addition to weakening the immune system and raising susceptibility to infections.
Early treatment of gingivitis and maintaining a consistent oral hygiene routine do more than protect your teeth—they are an essential part of preventing many chronic systemic diseases.
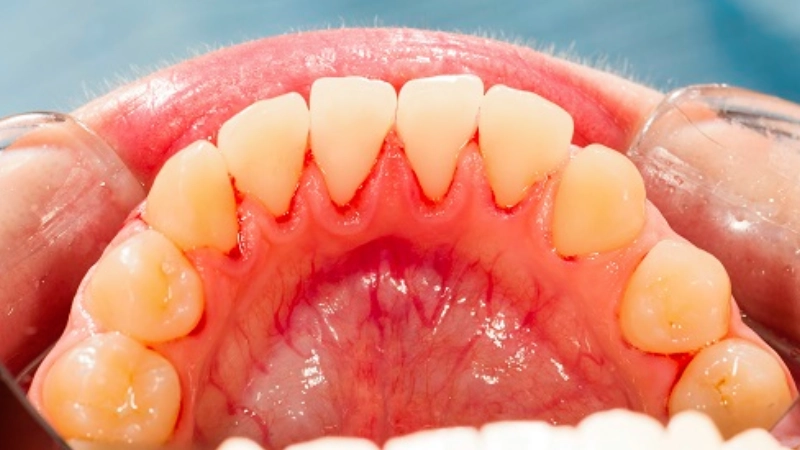
Conventional Treatment Methods for Gum Inflammation
Conventional treatment of chronic gingivitis relies on a set of dental procedures designed to eliminate the bacteria causing inflammation and to halt the breakdown of gum tissue.
Treatment typically starts with a deep professional cleaning of the teeth and gums (Scaling & Root Planing) to remove calculus (tartar) and hard deposits that have accumulated below the gumline, which are the main contributors to chronic gum inflammation.
The dentist may also prescribe topical or oral antibiotics to control gingival infection and reduce bacterial growth inside periodontal pockets, along with an antiseptic mouthwash containing chlorhexidine to help disinfect the mouth, reduce bleeding, and control bad breath.
In more advanced periodontal disease, minor surgical procedures may be required to reduce the depth of periodontal pockets and reshape the gums and the supporting bone around the teeth. This helps stabilize the teeth and limit further gum recession.
Consistent daily oral hygiene—such as brushing twice a day and using dental floss or interdental brushes—is an essential part of the success of conventional treatment and of maintaining healthy gums over the long term.
The Latest Laser Treatment Techniques and How They Work
Laser therapy is one of the most advanced and effective techniques for managing chronic periodontitis, relying on focused light beams that precisely target bacteria and inflamed tissues without damaging the surrounding healthy structures.
Gum laser treatment helps eliminate periodontal pockets and debride tooth roots, while significantly reducing bleeding and discomfort compared with conventional surgical procedures.
In addition, laser energy assists in disinfecting the affected area and stimulating tissue regeneration and reattachment of the gums to the tooth surface, which contributes to controlling chronic gum inflammation and improving tooth stability over the long term.
Modern laser-based periodontal therapies are characterized by short session times, reduced need for pain medication, and superior aesthetic outcomes, making them an advanced and safe option for treating gum disease and enhancing overall oral health.
Professional tips to prevent recurrent gum inflammation
To help prevent chronic, recurrent gingivitis, it’s recommended to brush your teeth at least twice daily using a soft-bristled toothbrush and fluoride toothpaste, taking care to gently clean along the gumline to remove dental plaque before it hardens into harmful calculus (tartar).
Daily use of dental floss or interdental brushes helps clean the spaces your toothbrush cannot reach, reducing the buildup of bacteria responsible for gum inflammation.
An antiseptic mouthwash recommended by your dentist is especially beneficial in cases of recurrent gum disease, as it helps reduce bacterial load and improves breath odor.
Smoking cessation is a key factor in preventing chronic gingivitis. Smoking weakens the immune response in the gums, impairs healing, and increases the risk of tooth loss.
Maintaining a balanced diet rich in vitamin C, vitamin D, and calcium supports the health of the gums and the bone surrounding the teeth. At the same time, limiting sugar intake and frequent snacking deprives oral bacteria of the nutrients they thrive on.
Regular dental check‑ups (every six months, or as advised) are also essential for comprehensive examination and professional cleaning to remove deep calculus and to treat any early signs of inflammation before they progress into recurrent chronic gum disease.
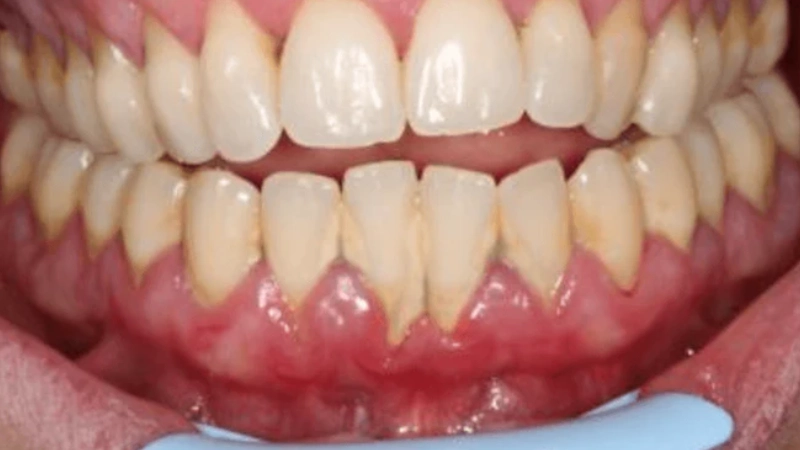
Chronic Gum Disease Treatment in Jeddah with Dr. Abeer
In Jeddah, Dr. Abeer offers a comprehensive treatment plan for chronic gum disease, starting with an accurate diagnosis based on clinical examination, radiographic imaging, and a thorough review of the patient’s medical history.
Management of chronic gingivitis and periodontitis typically includes deep cleaning of the gums and tooth roots (scaling and root planing) to remove tartar and bacterial plaque below the gumline. When needed, she may prescribe local or systemic antibiotics to help control the bacterial infection.
In more advanced periodontal cases, Dr. Abeer may perform minimally invasive surgical procedures to reshape the gums and the supporting bone around the teeth, with a strong emphasis on preserving the natural teeth whenever possible.
She also designs an individualized preventive program for each patient, which includes instruction on proper brushing techniques, the correct use of dental floss and medicated mouthwashes, along with regular follow‑up visits. This approach helps control chronic gum inflammation, reduces the risk of recurrence, and supports a healthy, attractive smile over the long term.

Frequently Asked Questions About Chronic Gingivitis
What is chronic gingivitis?
Chronic gingivitis is a long-term inflammation of the gum tissue caused mainly by bacterial plaque accumulation around the teeth. It often leads to symptoms such as swollen gums, bleeding during brushing, and persistent bad breath if not treated early.
What are the main symptoms of chronic gingivitis?
Red, swollen gums
Bleeding during brushing or flossing
Persistent bad breath
Gum tenderness or discomfort
Gum recession in advanced stages
What causes chronic gingivitis?
The most common causes include:
Poor oral hygiene and plaque buildup
Smoking
Diabetes
Hormonal changes
Vitamin deficiencies
Poorly fitted dental restorations
Can chronic gingivitis lead to tooth loss?
Yes. If untreated, chronic gingivitis may progress to periodontitis, a more serious form of gum disease that damages the bone supporting the teeth and may eventually lead to tooth loss.
Can laser therapy treat gum disease?
Yes. Modern dental lasers can remove infected tissue, eliminate bacteria, and stimulate gum healing with minimal bleeding and discomfort compared to traditional surgery.
How can chronic gingivitis be prevented?
Brushing teeth twice daily
Using dental floss daily
Regular dental check-ups
Avoiding smoking
Maintaining a balanced diet